On the Front Lines of the Covid-19 Battle
Cathi is a nurse who works on a Covid-19 Ward in a smaller Michigan hospital that normally has 300 beds. With the world facing the Covid-19 crisis, she is on the front lines of the battle to save lives, a battle that is lost far too often. Twists and turns in her life gave Cathi a later start to nursing, but she has been privileged to work at the same hospital her whole career and has witnessed how the practice of medicine has changed over the years. She is also approaching her 50s, in a career that has given her perspective on the effect that dealing with the Covid Virus has had on both patients and their loved ones.
Over the past 18 years, she has seen the operations at her hospital undergo an evolution. Cathi says, “When I started way back in 2002, we didn’t do any testing on the weekends. We didn’t do any radiology on the weekends. If you were remotely sick we sent you away [to a larger hospital]. Then we started adding some more cardio-vascular services. And we added a stress lab, cath lab. Patients that were traditionally sent to [a larger hospital] we were starting to keep.”
As her hospital gained certifications to do more and more procedures they found that, in cardiac care, in particular, they were able to excel. “ Our door to balloon times were half that of bigger hospitals,” she says proudly of the time it took a patient to arrive at the hospital and then receive an angioplasty. Eventually, the hospital gained permission to do a certain type of cardiac procedure on patients experiencing cardiac arrest. In the past, those cases would be sent to a larger, more specialized hospital, and would result in a delay of a few hours as the patient was transported and admitted. Now, Cathi’s hospital has been given permission to begin the procedure right away, on-site, while a specialist from the larger hospital is on call and goes to them. This cuts down wait times and saves significantly more heart muscle.
Cathi says, “That is supposed to be 90% of what we do. We have a generalized intensive care unit. We do kidney stuff, we do brain stuff, we do lung stuff…. We do brain drains for brain bleeds. We do dialysis Monday through Friday throughout the hospital.” While this may seem to be a natural evolution for a hospital to go through, it turned out to be a major benefit for the community as it has had to shift its resources to fighting the Covid-19 Pandemic.
Covid is completely different
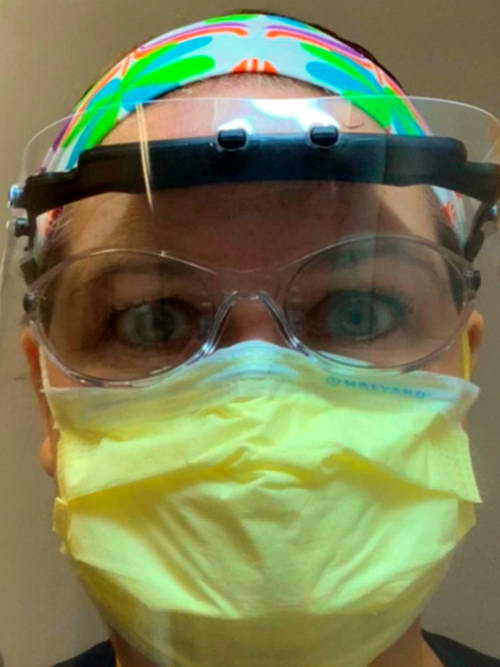
Cathi now finds herself on the front lines of a battle that is completely different from anything she has experienced before. The changes start right at the front doors of hospitals across the world. “What everyone is missing,” she says, “is that people are coming into the hospital but we aren’t allowing visitors because we don’t want them to get sick.” This means that people are not seeing the work that goes into helping Covid patients. “I work on a 30-bed unit; all but three or four rooms are Covid rooms or people under suspicion of Covid. There’s 30 isolation carts. There’s ten nurses, we have three patients each.” In order to treat the patients safely, the nurses are “donning and removing two facemasks. The N95 we keep on all the time. A surgical mask. A set of goggles. A face shield. Two sets of gloves, and a gown.
“Every. Single. Room,” she says for emphasis.
“So every time we go someplace else, we’re taking off and putting on. Thirty rooms of that. There are 10 of us. On top of that, there’s call lights and trips to the bathroom. There’s twice as many medications, anti-inflammatory agents, convalescent plasma, antiviral medication, pain medications that people are requiring. And it’s a three-minute gig to dress and undress. So six minutes for every [room].”
“[Covid-19] lives on surfaces. I’m wearing my surgical cap for 14 hours a day because I don’t want it in my hair and take it home. I leave my shoes outside and walk straight to the shower, and my clothes go right in a hot laundry tub.”
For the patients, life is even harder. Cathi explains, “These people that come into the hospital for two or three weeks, the only people they see are nurses and techs and PCAs (Patient Care Assistants). All [the patients] see is eyeballs. They are wearing a mask. I’m wearing all that garb. We can let them Facetime. A lot of nurses will let them put their phones in baggies and Facetime with the patient’s family so they can at least see each other. But they are stuck in that room. They can not leave that room while they are there, even if they are mobile. It’s like being a caged animal in a zoo.”
The disease itself is unique, moving in patterns not normally expected, and that the medical community finds hard to predict. One complication comes from the fact that many Covid-19 symptoms mimic the flu. Cathi says patients “come in, they have a sore throat and a cough. Some people lose their sense of taste or smell, and that’s their only symptom. Some people have tummy aches and have screaming diarrhea for four days and run a fever and they’re fine.” People who don’t get a Covid-19 test and just assume that they had the common flu are often a large problem. Cathi has observed cases where “they’ve been sick for a week and they’re starting to feel fine so they bring a meal over to their mom. Their mom gets sick, she ends up on a ventilator and dies.”
There is another variation to this story that Cathi is seeing all too often. “Respiratory-wise, it’s so strange. There are some people that come in and they look fine. Their oxygen saturation is 82%, 84%. Normal is 98%. They look fine. The average person would be gasping for air, but they are walking and talking. They don’t see anything wrong.
Couples come in that have been hanging out in the same household for a week and a half. One of them starts to feel worse. The husband brings the wife in, the wife is on one of our medical-surgical floors for three or four days, gets the oxygen, gets the treatment, and goes home. The husband, who comes in feeling ok, he ends up on one of the medical-surgical floors. His oxygen requirements go up. He transfers down to us, he’s on a bi-pap, the last bit before a ventilator, for two or three weeks and then he goes on a ventilator and he dies three days later. There’s no prediction.”
The Toll of Covid-19
Cathi pauses here for a moment and then begins to tell a story. Imagine a small business, like so many small businesses around the country. They are family-owned and passed down through succeeding generations. Employees are made up of family members and other hired staff. Often the founders of the business are retired, their kids now in charge of the legacy. Like any small group of people that works closely together, Covid-19 can take root. Cathi has seen it. The tragedy of it all was that even though all of the employees and kids recovered, someone unwittingly infected the retired founders, and it was one of them, unfortunately, who would not recover. That person died, Cathi points out with both sadness and anger in her voice, “because these people could not follow mask protocol and stay the frick away from each other!”
Cathi is quick to dismiss that Covid-19 is simply a bad flu. She has, after all, encountered many Influenza patients in her career. “The flu is mainly a respiratory disease,” she states. “Covid triggers your whole inflammatory cascade. It attacks your body. I’m seeing extra heart attacks and strokes. Things that may have happened in a few years, or gotten worse, speeding up that inflammatory cascade. People are ending up with kidney damage, with liver damage. It’s whatever system is more susceptible that is being affected. People are having heart attacks, people are ending up with heart failure. People are sick for so long. The first wave of this, we had people in our unit for a month, 6 weeks.
“It’s the scariest thing I have ever seen,” Cathi says softly. “You just never know. People will be doing great. You think they’re coming around and they just up and die. They have a fatal arrhythmia and you just aren’t going to get it back. People just all of a sudden… We had a patient the other day who said, ‘I think this is going to be my last day on earth,’ and sure enough… he seemed to be coming around and doing better, you know.”
You can hear the frustration in Cathi’s voice as she continues, “Forgive me, this is oversimplifying. People with chronic illnesses get to say, ‘You know, I feel like I don’t want to do this anymore. I think the next time it happens I just want to be made comfortable.’ [With Covid-19] you have someone who has been in the hospital for three weeks and they have to be put on a ventilator.
“They aren’t sick–sick, they just can’t breathe. They feel awful. They can’t manage to get off the bi-pap mask to take a sip of water or get something to eat. They are getting their nutrition through a tiny tube down their nose or through their IV. It’s too exhausting just to chew, but their brain is there. Three weeks ago, they were mowing the lawn, and cleaning out their garden, and riding the tractor with their grandkids. Now it’s too much effort to even hold a glass of water without feeling like they are going to die because they are so short of breath.”
Covid-19 is often not a “normal” experience, either for the patient or their loved ones. “That’s what people don’t get. Their family member came in three weeks ago and were fine. [The patient] chatted with you on the phone for the last few weeks, seemed to be fine on the mask. But I know, [the patient is] on 70, 80, 90% oxygen. Pushing it like a CPAP or a BiPAP, pushing air into your lungs so that the stiff lungs can open up and breathe.”
The end, Cathi says, often comes unexpectedly. “When I call and say ‘There’s not much more that I can do for your dad, I’m going to have the doctor talk to you. I think it’s time for you to come in because you guys have to have a serious discussion,’ [the patient’s family members] are surprised because they missed that in-between stuff where you can come in and you get to hold hands and you get to grieve.”
Covid-19 is brutal. “These people are gasping for air, and the doctor is telling them, ‘This is as much oxygen as I can give you without putting you on a ventilator. If I put you on a ventilator, you’re not going to ever get off of it. You’re probably not going to survive. What do you want to do?’” Some patients have had enough and ask to be put to sleep, to be put on a ventilator, to be made comfortable and allowed to die.
Once that process is started, Cathi says, there is a protocol that must be followed. “Okay, so you decide to do that. Then I can let 2 of your family members come in – two of them.
“And they can don full gear like I have on.
“And they can watch from outside the window as I hold your hand and you die.”
Waiting for the pandemic to end
Cathi is not political, not trying to prove a point other than the fact so much of this is preventable. “90% of the people with Covid are still at home, and they are still infecting the people around them, and still infecting their communities. That is why it hasn’t gone away. It’s as simple as just staying the hell away from each other. And not being angry, and not hiding your symptoms.
“It’s not just old people,” Cathi continues. “It’s couples, 50s, 60s, middle-aged men getting sick. They still go to work, they still go to the grocery store. They still go in and out of gas stations. Older people, 70s, and 80s can stay home. It’s their kids infecting them. “
Cathi does note an irony to the complaining she hears about mitigation methods, particularly those that limit gathering size. “It mirrors what electronics have done to us anyways. Our relationships have become electronic, they have become over the phone or over the internet. That’s how you meet people now, that’s how you hang out with people now. That’s the ironic thing! They are bitching about not being able to see each other when in reality people don’t see each other anyway!”
Because of her profession, Cathi has seen more than her share of death in her career. Covid is simply increasing the numbers at a faster pace. It is tragic, and yet there are moments of beauty within the tragedy, too.
Cathi recently had a patient, an older gentleman who always had a smile and a joke for her. She said, “every time I would walk in I’d say, ‘Hey! Tell me a joke!’ This was a fella that had had twelve hip surgeries. Over the span of 2 years–twelve hip surgeries! Three weeks later [after his final surgery] he gets Covid, leaving his poor little frail wife at home alone with Covid, and his daughter to take care of her. He’s stuck in the hospital for three and a half weeks.
“Eventually he was moved down to the unit where I normally work. I stopped in to see him and joke with him. ‘Oh, it’s you! I was meaning to see you. I wanted to chat with you’. We got caught up over the last week or so, and then I had three or four days off”.
When Cathi returned to the Hospital after her time off, the patient was gone – he had died suddenly. Cathi was dumbfounded. “I was like – What? He was doing great!”
Her patient, though, had accepted his fate and used his final days well.
“He had known that he was getting worse and was on more and more oxygen. He got on his phone and he recorded personal messages for Christmas for each one of his grandkids, for each of his kids, his daughter-in-law, and this huge video message to his sweet little wife who couldn’t be there before he decided to take himself off of oxygen and died.
“I cried my eyes out. I cried and cried and cried and cried and cried. And cried all the way home from work. It was so beautiful, he was so at peace because the Lord was his Savior. He had found God after 20 years of doubting himself. I think all along in those three weeks that he knew what was happening. He decided to rejoice at the end of his life.”
Cathi believes that we all have a prewritten story which we live out and it is her faith that there is a larger purpose that keeps her going. Nursing, and the Pandemic, in particular, have taken a toll on her physically and mentally. “It’s probably the only way I can get through every single day doing this. I’m just part of the plan. If the Lord wants to bring you home, then the Lord is going to bring you home.” She takes comfort in her belief that her job is to do the best she can for each and every patient, but the ultimate outcome is in the hands of a higher power.
Cathi can not wait to celebrate the day when this pandemic is finally in the history books. A day that will come sooner the more people understand and accept the role that they play in the mitigation strategies found in every community. “This isn’t fair,” Cathi says quietly. “What these people are going through isn’t fair. 90% of the people with Covid are still at home, and they are still infecting the people around them and still infecting their communities. That is why it hasn’t gone away. It’s as simple,” she says, “as just staying the hell away from each other and not being angry and not hiding your symptoms.”
Interview conducted December 2020
Headshot courtesy of Cathi





0 Comments